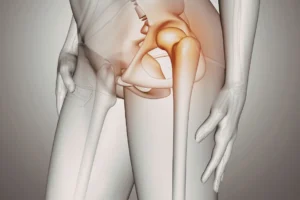
Espondilitis Anquilosante: No dejes que el dolor de espalda te fusione

Ankylosing Spondylitis: Don’t Let Back Pain Fuse Your Spine
If you feel persistent pain in your lower back or in your hip, a type of discomfort that worsens when you rest and forces you to wake up stiff in the morning, you need to pay very close attention. This type of pain is not the typical mechanical pain that disappears with rest; in fact, it is quite the opposite. This pattern of discomfort suggests chronic inflammation that could be Ankylosing Spondylitis (AS).
Ankylosing spondylitis is a progressive autoimmune disease that, if not treated in time, can lead to the fusion of the vertebrae, turning your spine into a rigid and limiting structure. This is what is commonly known as a bamboo spine.
It is essential for you to understand that time is critical. Every day of untreated inflammation is a step toward permanent stiffness. Therefore, if you identify with the symptoms I will describe below, it is urgent to seek a specialized evaluation.
What Is Ankylosing Spondylitis?
Ankylosing spondylitis is a chronic inflammatory rheumatic disease. It belongs to the group of conditions known as spondyloarthritis. Its main characteristic is that it primarily affects the sacroiliac joints (where the spine connects to the pelvis) and, progressively, the spine.
Imagine that your joints are hinges that allow movement. In ankylosing spondylitis, your own immune system, for reasons that are not yet fully understood, begins to attack these hinges. This constant inflammation causes pain and, over time, the body attempts to heal this inflammation by depositing calcium and new bone. The result is ankylosis, which means fusion or consolidation.
When the vertebrae fuse, you lose flexibility and mobility. This not only affects your back, but it can also impact your posture, your breathing capacity, and, importantly, peripheral joints such as the hips and shoulders. Therefore, it is a systemic disease that requires comprehensive management.
Symptoms That Indicate Ankylosing Spondylitis
It is vital to differentiate mechanical pain (caused by strain, posture, or wear) from the inflammatory pain that characterizes ankylosing spondylitis. Pain caused by AS has very specific characteristics that will help you recognize the seriousness of your situation. In addition, remember that this disease usually manifests in young individuals, generally before the age of 45.
Lower Back and Sacroiliac Pain
The initial and most common symptom is pain in the lower back and in the gluteal region, which corresponds to inflammation of the sacroiliac joints (sacroiliitis). This pain is not constant, but instead follows a very clear pattern:
- It worsens with rest, especially at night or at the end of the day.
- It wakes you up in the second half of the night, forcing you to get up and walk to relieve it.
- It improves significantly with exercise or physical activity.
- If your back pain improves when you move, do not ignore it. This is a major warning sign that requires immediate evaluation.
Prolonged Morning Stiffness
Stiffness upon waking is another diagnostic cornerstone. If you wake up feeling your back or neck completely stiff, and this sensation takes more than 30 minutes (sometimes several hours) to subside, we are dealing with inflammatory stiffness. In contrast, stiffness caused by mechanical wear usually lasts only a few minutes.
This stiffness limits your ability to perform simple tasks, such as tying your shoes or turning your head. In addition, as the disease progresses, stiffness can become permanent due to bone fusion.
Involvement of Other Areas of the Body
Ankylosing spondylitis is not limited to the spine. In fact, it can manifest in other areas where tendons and ligaments attach to the bone, a phenomenon known as enthesitis. For example, you may experience pain in the Achilles tendon, in the sole of the foot (plantar fasciitis), or in the ribs, causing chest pain.
Additionally, approximately one-third of patients develop arthritis in peripheral joints, with the hips and knees being the most affected. If inflammation destroys the hip joint, joint replacement surgery may be necessary. Other symptoms include eye inflammation (uveitis), chronic fatigue, and, in rare cases, heart or lung problems.
Causes of Ankylosing Spondylitis: Genetic Predisposition and Immune Response
Although ankylosing spondylitis does not have a single known cause, we know that it has a strong genetic component. It is not a wear-and-tear disease, but rather an error in the programming of your immune system.
The most important genetic factor is the presence of the HLA-B27 gene. While not all individuals with this gene develop ankylosing spondylitis, the vast majority of diagnosed patients have it. Therefore, if you have first-degree relatives with AS, your risk increases considerably. The HLA-B27 gene appears to make the immune system more susceptible to being activated by environmental factors or by intestinal or urinary infections. Once activated, the inflammatory process becomes chronic and attacks the skeletal joints.
The Diagnostic Process
The diagnosis of ankylosing spondylitis requires a combination of medical history, physical examination, and imaging studies. Because the initial symptoms are subtle, there is often a delay of several years in diagnosis, which is unacceptable given the progressive nature of the disease.
The first step is an evaluation by a specialist, looking for signs of limited movement, such as the ability to flex the spine (Schober test) or hip mobility. In addition, palpation of tendon insertion points is crucial.
Key Imaging Studies
- X-rays: Plain radiographs are essential to detect structural changes. In advanced stages, they show spinal fusion (bamboo spine). However, in early stages, we specifically look for signs of sacroiliitis (erosions, sclerosis, or fusion) in the sacroiliac joints.
- Magnetic Resonance Imaging (MRI): MRI is the most sensitive study for early diagnosis. It is the only tool that allows us to detect active inflammation (bone marrow edema) before structural damage becomes visible on X-rays. If we suspect ankylosing spondylitis, an MRI of the sacroiliac joints is mandatory.
- Blood tests We look for inflammatory markers such as erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP). In addition, HLA-B27 testing helps confirm genetic predisposition, although a negative result does not rule out the disease.
Modern Treatment to Preserve Your Mobility
The primary goal of ankylosing spondylitis treatment is to control inflammation, relieve pain, maintain mobility, and prevent bone fusion. This is a condition that requires lifelong management, and collaboration between the rheumatologist and the orthopedic surgeon (for joint-related complications) is essential.
Conservative Treatment: Exercise as Medicine
Physical activity is not optional; it is a cornerstone of treatment. Rest, in fact, worsens stiffness. Therefore, therapeutic exercise must be consistent and focused on maintaining flexibility and proper posture. Specialized physical therapy will help you:
- Improve range of motion in the spine and hips.
- Strengthen postural muscles to prevent kyphosis (forward curvature).
- Maintain lung expansion capacity, which can be affected by rib fusion.
- Nonsteroidal anti-inflammatory drugs (NSAIDs) are also used in controlled doses to manage pain and reduce inflammation, allowing the patient to exercise effectively.
Advanced Pharmacological Treatment
If NSAIDs and physical therapy are not sufficient to control the disease, treatment must be escalated. This is where modern rheumatology has made extraordinary progress. The use of biologic therapies has dramatically changed the prognosis of ankylosing spondylitis.
- Disease-modifying antirheumatic drugs (DMARDs):Medications such as sulfasalazine are often used, especially when peripheral joints (knees, hips) are involved.
- Biologic therapies: These are highly targeted medications that block specific inflammatory pathways, such as tumor necrosis factor (anti-TNF) or JAK inhibitors.
Surgical Intervention for Structural Damage
Although surgery does not cure ankylosing spondylitis, it becomes necessary when the disease has caused severe structural damage or disabling deformities such as:
- Spinal deformities (severe kyphosis):If the spine has fused in a significantly forward-bent position, preventing the patient from looking straight ahead or affecting quality of life, spinal osteotomies are performed. These are highly complex procedures in which the fused spine is cut and realigned to restore balance and posture. It is major surgery, but it can restore lost function.
- Peripheral joint destruction: Ankylosing spondylitis is particularly aggressive in the hip joint. If chronic inflammation has destroyed cartilage and bone, causing severe pain and functional limitation, the solution is total hip arthroplasty (hip replacement surgery). This surgery is highly effective in relieving pain and restoring hip movement, even in young patients with AS.
Living Without Pain Is Possible: Stop the Progression of Ankylosing Spondylitis
Ankylosing spondylitis is a serious disease, but it is no longer synonymous with disability. Today, with advances in biologic therapies and expert orthopedic management, it is possible to live a full and active life. However, this requires early diagnosis and strict adherence to the treatment plan.
Do not accept chronic lower back pain or morning stiffness as something normal or simply part of aging. If your pain improves with movement and wakes you up at night, you are losing valuable time. You need an evaluation to confirm or rule out ankylosing spondylitis and to stop the progression of the disease.
If you suspect that you have ankylosing spondylitis, or if you already have a diagnosis but feel that your current treatment is not sufficient, it is time to act. Schedule your consultation. Together, we will define the most modern and effective strategy to preserve your joints and prevent spinal fusion. Do not wait until stiffness becomes permanent.

Dr. Raul Lopez Solis
Hip & Knee Surgeon
Professional License: 926463 / Health Ministry Registry (SSA - Mexico): 2204 / Specialty License No.: AESSA-27436
Facebook: Dr Raul López Orhtopedic Surgeon
Instagram: drraullopezs
TikTok: @drraullopezs
Web site: About me